Are you considering a cosmetic procedure but wondering if your insurance might help with the cost? Many people assume that cosmetic surgeries are entirely out-of-pocket, yet in specific medical circumstances, some treatments may qualify for insurance coverage. While purely aesthetic procedures rarely receive approval, surgeries or treatments linked to health conditions, injuries, or physical discomfort can sometimes be reimbursed. Understanding these distinctions can help you save thousands and make informed decisions about your care. In this article, we explore the top five cosmetic procedures that might be covered by insurance and explain the medical reasons that make them eligible. Knowing your options can empower you to pursue both wellness and confidence without unnecessary financial strain.
Rhinoplasty (Nose Surgery)
Rhinoplasty is widely known for reshaping the nose to improve appearance, but in certain cases, it’s considered a medically necessary procedure. Insurance may cover part or all of the cost if it corrects breathing issues, such as a deviated septum or nasal deformity caused by trauma. Patients who experience chronic nasal obstruction or sleep-related breathing problems may qualify after proper evaluation by an ear, nose, and throat specialist. The key factor is documentation — your doctor must provide detailed medical evidence that the surgery improves function rather than simply alters appearance. Combining functional correction with cosmetic adjustments is common, but only the medically required portion is typically covered by insurance.
Breast Reduction Surgery
For many women, overly-large breasts cause significant discomfort — including chronic back, neckand shoulder pain, skin irritation, or posture problems. In such cases, breast reduction surgery can shift from a cosmetic choice to a medically necessary intervention. Insurance companies often review physical symptoms, medical history, and even photos to assess the need. Some may require proof that other treatments, such as physiotherapy or pain management, have been tried unsuccessfully. If approved, the procedure can bring tremendous relief and boost self-esteem. It’s one of the few cosmetic surgeries with strong potential for insurance reimbursement when health concerns clearly outweigh aesthetic goals.
Eyelid Surgery (Blepharoplasty)
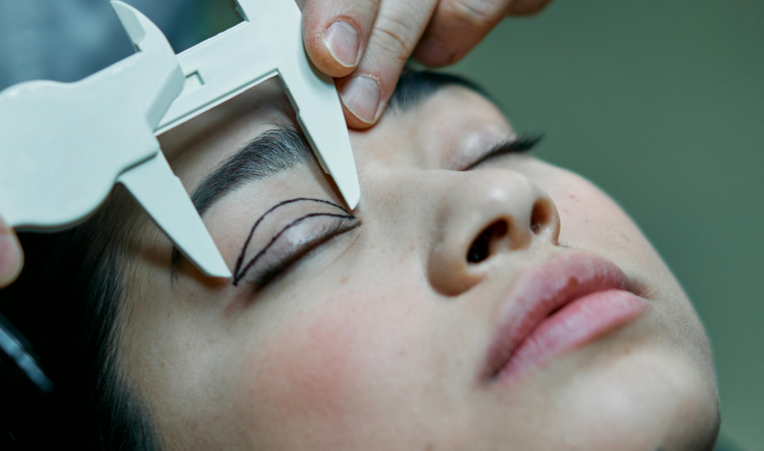
While eyelid surgery is commonly performed to rejuvenate appearance through removing excess skin or fat around the eyes, it can also serve a medical purpose. In some individuals, drooping eyelids — known as ptosis — can obstruct vision, making daily activities difficult. Insurance coverage becomes possible if an ophthalmologist documents that the sagging skin interferes with sight. Functional blepharoplasty helps restore normal vision and reduce eye strain, particularly in older adults. However, surgeries done purely for cosmetic tightening or symmetry will not qualify. Proper diagnosis and medical photography that demonstrate the impact on vision are usually required for insurance approval.
Reconstructive Surgery After Injury or Illness
Reconstructive procedures are among the most frequently covered cosmetic-related surgeries, especially those following accidents, burns, or medical conditions like cancer. For example, breast reconstruction after a mastectomy, skin grafts for severe burns, or scar revision surgeries often qualify for full or partial coverage. These procedures help patients restore appearance and function lost due to trauma or illness. The difference lies in medical necessity: if the surgery repairs or restores damaged tissue rather than enhancing features for aesthetic preference, insurance is likely to assist. Documentation from a specialist and clear medical justification are essential to strengthen your claim.
Skin Removal After Significant Weight Loss
After major weight loss — especially from bariatric surgery — excess skin can cause discomfort, hygiene problems, and infections. In such cases, procedures like a panniculectomy (removal of skin from the lower abdomen) might be deemed medically necessary. Unlike a tummy tuck, which focuses on contouring, a panniculectomy targets excess skin that causes physical issues. Insurance providers often require proof of recurrent rashes, irritation, or physical limitation caused by the hanging skin. If approved, patients can experience both functional relief and improved mobility, making this procedure one of the few cosmetic-related surgeries covered under specific conditions.
While most cosmetic procedures remain elective and self-funded, several exceptions exist where insurance coverage becomes possible due to medical necessity. Surgeries like rhinoplasty for breathing correction, breast reduction for pain relief, eyelid repair for vision obstruction, reconstructive surgery after trauma, and skin removal after weight loss can all qualify with proper medical documentation. The process requires patience and communication between patients, physicians, and insurance providers. Understanding the criteria before committing to a procedure can save both time and money. By approaching these decisions with clarity and verified information, individuals can achieve their health and aesthetic goals responsibly and affordably.